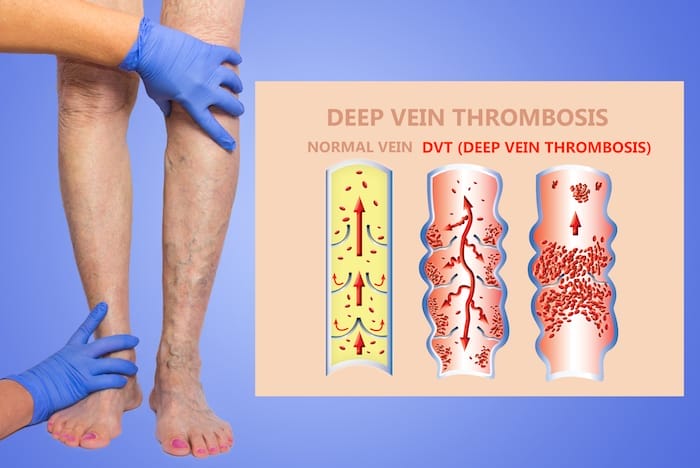
Deep vein thrombosis can be a serious or even deadly condition. It can arise from different situations. For example, if you break a bone in a car accident or a similar situation, it can actually cause DVT. DVT can then turn into a pulmonary embolism.
Other things that can cause DVT include surgery, limited movement, some medications, and veins.
Specific risk factors often linked to DVT are:
- Having an inherited blood clot disorder
- Being on extended bed rest, for example, if you’re in the hospital
- Pregnancy
- Birth control pills
- Hormone replacement therapy
- Being overweight or obese
- Smoking
- Some types of cancer
- Heart failure
- Inflammatory bowel disease
- Being older than 60
- Sitting for long periods
So what else should you know about this condition?
What is DVT?
DVT is caused by a blood clot located in a deep vein. Symptoms include pain, tenderness, and swelling in the legs.
When blood moves through slow through the veins, it can lead to a clump of blood cells, which is a clot. Again, when that clot is in a vein located deep inside your body, it’s DVT. These clots are most likely to occur in your thigh, leg, pelvis, and lower leg. They can occur in other parts of the body too.
Along with pain or swelling, signs of DVT can also include enlarged vein and skin that looks blue or red.
If you have a blood clot that breaks free and moves through the bloodstream, it can get stuck in a lung blood vessel. This is a pulmonary embolism, which can be deadly.
DVT Complications
There are certain complications of DVT to be aware of. One was mentioned, which is pulmonary embolism or PE.
If a blood clot breaks off and travels to the lung, it can cause serious lung damage. If the clot is large, it can prevent blood from reach the lungs, and it can be deadly.
Signs and symptoms of pulmonary embolism including problems breathing, irregular or fast heart beat, chest pain, coughing up blood, or low blood pressure.
There can also be a complication called post-thrombotic syndrome or PTS that occurs.
If you have PTS, symptoms can include swelling, discoloration, and pain. In severe instances, PTS can lead to scaling or ulcers in the areas of the body affected. PTS occurs when the clot damages the valves in the vein. In some cases, when it’s very severe, the condition can lead to disability.
Both DVT and PE have the potential to become chronic illnesses as well. It’s estimated that around 30% of people who have DVT or PE are at risk for it happening again.
Can You Prevent DVT?
There are certain things you can do, dependent upon your specific situation, to reduce the risk of DVT.
For example, if you are injured or have surgery, as soon as you’re safely able to do so, try moving around.
If you know that you’re at risk of DVT, you might also speak to your doctor about whether or not to wear medical compression stockings.
If you sit for long periods of time, such as at a desk or on a plane, try to get up and move and walk around every couple of hours, at least.
If you’re sitting, raise and lower your heels while your toes remain on the floor, and tighten and release your leg muscles.
You can also avoid a sedentary lifestyle and work to maintain a healthy weight.
Are There Treatments for DVT?
A doctor can diagnose PE or DVT using certain tests. If you even suspect you have DVT, you should speak to your doctor right away.
If you are diagnosed with DVT, medication and compression stockings are two of the main treatments used. If you wear compression stockings at the advice of your doctor, they might need to be worn for at least two years after the DVT. In very severe cases, a clot might have to be removed surgically.
For someone with PE, medical attention is needed right away. If someone has life-threatening or severe PE, there are medicines sometimes used to dissolve the clot. These medicines are called thrombolytics.
There are also anticoagulants that can prevent more clots from forming. Some people have to take anticoagulants for the long-term.
If you are older, are injured, or have certain medical conditions and you notice odd symptoms such as swelling or warmth in an area like your leg, you should speak to your doctor. It could be a DVT.
Senior Outlook Today is your go-to source for information, inspiration, and connection as you navigate the later years of life. Our team of experts and writers is dedicated to providing relevant and engaging content for seniors, covering topics such as health and wellness, finances, technology and travel.